Wed, Apr 24, 2024
Volume 29, Issue 3 (6-2019)
JHNM 2019, 29(3): 137-144 |
Back to browse issues page
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Amouei Foumani S, Paryad E, Ghanbari Khanghah A, Kazemnezhad Leili E. Complications of Peripheral Intravenous Catheters During 72 Hours After Insertion. JHNM 2019; 29 (3) :137-144
URL: http://hnmj.gums.ac.ir/article-1-1075-en.html
URL: http://hnmj.gums.ac.ir/article-1-1075-en.html
1- Nursing (MSN), School of Nursing and Midwifery, Guilan University of Medical Sciences, Rasht, Iran.
2- Instructor, GI Cancer Screening and Prevention Research Center (GCSPRC), Department of Nursing, School of Nursing and Midwifery, Guilan University of Medical Sciences, Rasht, Iran , e_paryad@gums.ac.ir
3- Associate Professor, Department of Nursing, School of Nursing and Midwifery, Guilan University of Medical Sciences, Rasht, Iran
4- Associate Professor, Bio-Statistics, Social Determinants of Health Research Center (SDHRC), Guilan University of Medical Sciences, Rasht, Iran
2- Instructor, GI Cancer Screening and Prevention Research Center (GCSPRC), Department of Nursing, School of Nursing and Midwifery, Guilan University of Medical Sciences, Rasht, Iran , e_paryad@gums.ac.ir
3- Associate Professor, Department of Nursing, School of Nursing and Midwifery, Guilan University of Medical Sciences, Rasht, Iran
4- Associate Professor, Bio-Statistics, Social Determinants of Health Research Center (SDHRC), Guilan University of Medical Sciences, Rasht, Iran
Full-Text [PDF 445 kb]
(877 Downloads)
| Abstract (HTML) (2664 Views)
Full-Text: (899 Views)
Introduction
Peripheral Intravenous (PI) line or venipuncture is widely used for the treatment of millions of patients around the world [1]. Injections of drugs, liquids, blood products, and Intravenous nutritional supplements are the most important use of these catheters [2]. About 70% of patients need at least one PI catheter after hospital admission, and about 200 million catheters are used per year in the U.S. [3]. But this method is not entirely safe and has some complications. One of these complications is phlebitis which may be present in 50% of the patients in general and up to 75% in patients with infectious diseases, but in patients with no diabetes, burns, or catheterization in emergencies, the incidence is approximately 20% [4].
Phlebitis can be dangerous because it causes clot formation within veins and occurrence of thrombophlebitis and, in some cases, embolism [5]. Another serious complication is sepsis, which occurs in about 1% of cases [3, 6, 7]. Other complications such as drug and fluid leakage, occlusion, and local infection may also be observed [6].
These complications may occur at various stages, during the initial assessment to find the appropriate site for catheterization or subsequently during catheter insertion or maintenance of catheter placement. Several factors affect the incidence of these complications such as aging, gender, vein selection, equipment selection, disease process, treatment protocols, and the skill of the person who performs venipuncture [8].
Catheter site and indwell time are also related to the incidence of complications, especially phlebitis [1, 8, 9]. Hence, although it may take up to one week or even more for catheters and Intravenous fluid administration, they are usually replaced in shorter intervals to minimize the complications [3]. The recommended time interval for routine replacement of catheters has been increased over the past three decades from 24 to 48 hours and then to 72 hours [6]. In some recent nursing studies, the recommended time line is 72 hours [10-12]. In spite of this recommendation, complications sometimes occur sooner. Thus catheter replacement is necessary, and sometimes it is replaced in 72 hours without a complication. The Centers for Disease Control and Prevention (CDC) has recommended this time to every 72-96 hours [13].
The nursing team is responsible for PI catheter insertion and care [14]. Therefore, the determination of complications and their frequencies extent are necessary for nursing care. In this regard, a study conducted in Turkey showed that the incidence of phlebitis in catheterizations, which were in place less than 48 hours, was significantly higher than that of other time durations [9]. Another study on patients admitted to the general surgery department showed that the lowest rate of phlebitis was related to 0-24 h timeline [15].
Results of a prospective cohort study in five Italian hospitals indicates that with every 24 h increase in catheter indwell time, the likelihood of phlebitis increases by 5% [1]. While in a retrospective study on the patients hospitalized in a surgical department in the U.S., no difference was reported between complications of catheters indwelled for 72-96 hours and those remained for more than 96 hours [16].
Considering the wide range of factors affecting the complications of PI catheters and the different results regarding the incidence of these complications, further studies are needed to examine the situation and revise the current guidelines. In this regard, this study aimed to investigate the incidence of complications of PI catheterization within 72 hours after insertion.
Materials and Methods
This is an analytical cross-sectional study design conducted on the patients hospitalized in cardiac surgical wards of an educational treatment hospital in Rasht City, Iran after undergoing Coronary Artery Bypass Graft (CABG) operation. These wards were selected because the patients received the same antibiotics after CABG operation. The point is that the injection of some medications can exacerbate the complications of the injection site vein.
The inclusion criteria for the study patients were as follows: needed PI catheter for at least 72 h; had no peripheral vascular diseases (based on the medical records); not received immunosuppressive drugs (based on the medical records); lacked blood infection (based on the medical records), sensitivity to penicillin and antibiotics based on the routine surgical protocol, valvular heart disease; received the same Intravenous (IV) drugs; lacked allergy to adhesive or medical equipment (based on the medical records); and were interested to participate in the study. On the other hand, the exclusion criteria were as follows: change in the type of IV drugs taken during the study, blood transfusion, skin reaction to dressing adhesive on the catheter, and unwillingness to participate in the study.
According to the study of Salgueiro-Oliveira et al. where the rate of phlebitis was reported 11.09%, a sample size of 154 was determined, and the patients were gradually included in the study based on convenience sampling method [17]. Of 289 patients, 117 did not meet the inclusion criteria: 1 for unwillingness to participate; 75 for not receiving the same IV drugs; 7 for sensitivity to penicillin and thus, not receiving antibiotics based on the routine protocol of the surgical ward; 12 for having peripheral vascular disease; 16 for having valvular heart disease; 1 for receiving immunosuppressive drugs and not receiving the same IV drugs; 1 for having a history of allergy to adhesive tape; 1 for having both valvular heart disease and peripheral vascular disease; 1 for having peripheral vascular disease and not receiving the same IV drugs; and 2 for having PI catheters with different sizes. Of 172 remained patients, 4 patients were excluded as their information about catheter removal was not recorded; 7 patients due to change in the received IV drugs, and 7 patients because of blood transfusion. Thus the information of 154 patients was statistically analyzed.
The data collection tools were phlebitis assessment and infiltration rate scale developed by Infusion Nurses Society (INS) which were mentioned as standard tools to evaluate catheter insertion site in reference Nursing textbooks [5]. The phlebitis assessment scale has been rated from 0 to 4 (0=No signs of phlebitis, 1=pain on the insertion site with erythema or edema, 2=formation of streaks, 3=palpable venous cord with a length of more than 2.5 cm, and finally 4=purulent drainage). The Infiltration rate scale also has a grading scale of 0 to 4 from no sign to white, pale, and semi-translucent skin, tight and leaking skin, swollen and bruised skin, gross edema >15 cm in each direction, deep pitting tissue edema, impaired blood circulation, moderate to severe pain, infiltration of some blood products, and skin irritation and tenderness. Other tools included a form of personal, clinical, and catheter information.
From the beginning of the sampling, the medical records of the patients, who were transferred from the cardiovascular Intensive Care Units (ICUs) to the surgical wards and received new PIs, were investigated in terms of inclusion criteria every day. Each eligible patient was entered into the study only once, and if his or her catheter were removed and replaced with another one, the patient would not be re-entered into the study. In the ICU and during the transfer of the patient to the surgical ward, ICU nurses performed venipuncture according to the conventional method (preparation of the skin with 70% ethanol and fixing the catheter with an IV dressing which is a ready-to-use dressing for the catheter site with an anti-allergy adhesive).
20-Fr catheters (made by B. Braun Medical Inc., Pink color) were used for all patients. The personal, clinical, and catheter information form was completed for each patient and put into his or her medical file. The assessment tools for data collection were also put in each patient’s medical record to help the nurses use them when specifying the reasons for catheter removal. It should be mentioned that before the beginning of the study, the nurses of surgical departments were trained on how to use the study tools and they were asked to use a flexible ruler to measure the edema caused by IV drug infiltration. In case of occlusion of the catheter by a clot, first, they were supposed to aspirate the residual clots from the catheter by a syringe, and in case of failure, remove the catheter. In each working shift, the catheters were examined by the nurses regarding the signs of complications. Whenever the nurses saw any signs of complications, they removed the catheter and recorded the reason and time of removal in the related form.
This study was first approved by the Research Ethics Committee of Guilan University of Medical Sciences (Code: IR.GUMS.REC.1394.51) on May 30, 2015. Then, sampling started from July 28, 2015, and ended on March 18, 2016. The study purpose and procedure were explained to the patients, and written informed consent was obtained from them. They were assured of the confidentiality of their information and were free to leave the study at any time.
The obtained data were analyzed in SPSS V. 22. Descriptive statistics (frequency, mean, and standard deviation) were used for describing the individual characteristics, factors associated with the disease and the characteristics of the catheters. Inferential statistics (Fisher’s exact-test and the Chi-squared test) were used to investigate the effects of complications based on the above data.
Results
Our study results showed that most participants were male, aged over 60 years, and had a BMI of 25-30 kg/m2. Their most common underlying disease was hypertension, followed by hyperlipidemia. Most of the subjects were receiving non-Intravenous anticoagulant drugs (Aspirin, Clopidogrel, Enoxaparin, Warfarin). The most frequently used catheter site was antecubital, and the least frequent site was arm. The indwell time of most of the catheters was 49-72 h; the Mean±SD indwell time was 62.05±24.93 h (Table 1).
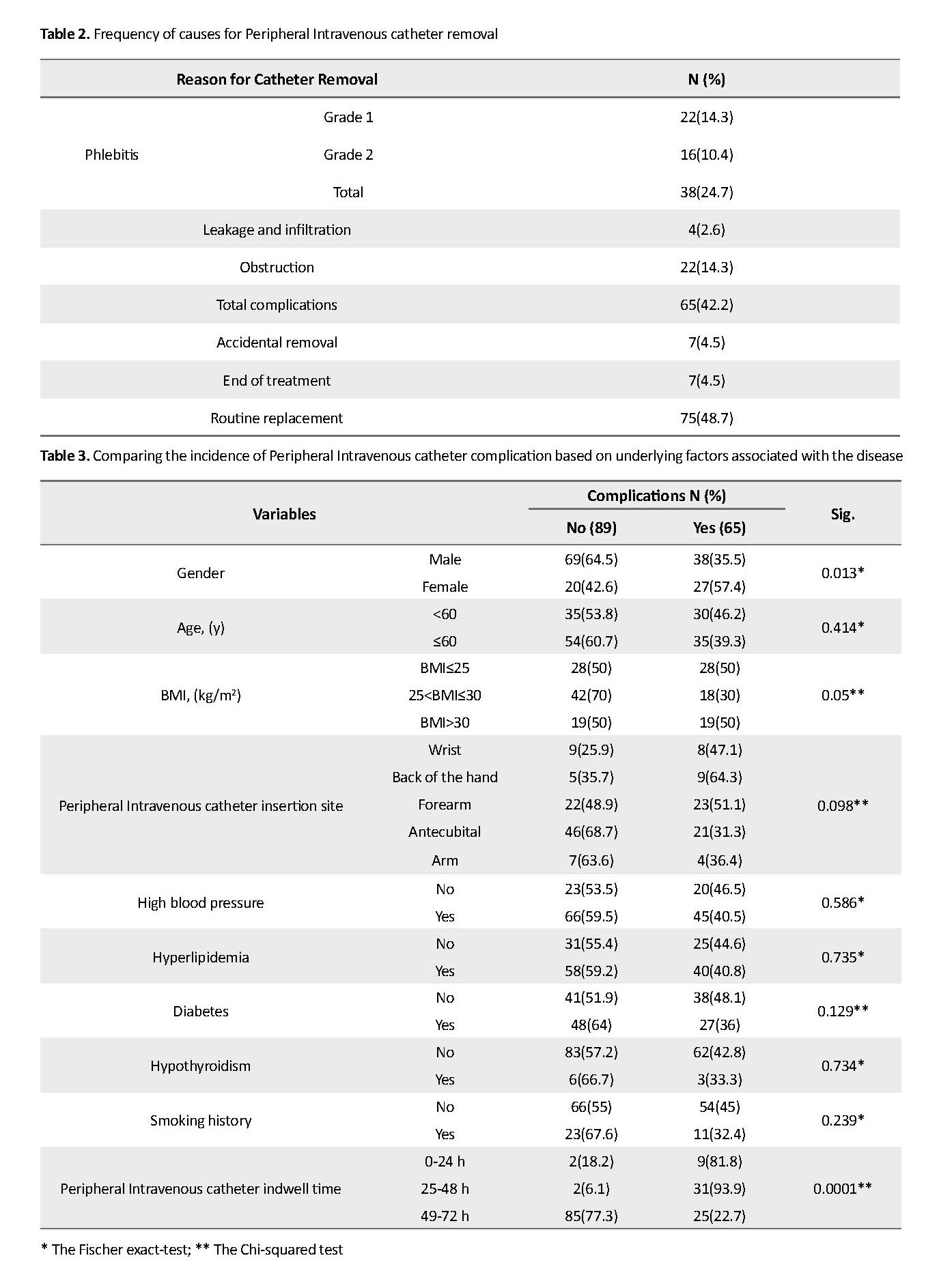
Based on the results, 48.7% of patients showed no sign of complications in the catheter site during the first 72 h. After 72 h, catheter replacement was performed according to the instructions of the hospital. About 42.2% of the catheters were removed due to the occurrence of at least one complication where the most common complication was phlebitis followed by an obstruction, drug leakage outside of the catheter, and then drug leakage into the patient’s tissue. Most cases of occurred phlebitis were grade 1 and then grade 2; no patient was observed with grade 3 or 4 phlebitis. All cases of leakage into the tissue were of grade 1 phlebitis (Table 2).
Complications in women were more than men, and the most complications occurred in the period of 25 to 48 hours after the catheterization and the least in the time range of 49 to 72 hours later (22.7%). The results reported a significant relationship between the incidence of complications associated with PIs and gender (P=0.013), indwell time of catheter (P=0.0001), and BMI (P<0.05) (Table 3).
4. Discussion
The results of the current study showed that the most reported complication associated with PI catheterization was phlebitis (grade 1). In the studies of Uslusoy and Mete, and Powell et al. where the measurement scales were similar to those used in the present study, the most commonly reported complication was grade 1 phlebitis as well [15, 18].
Peripheral Intravenous (PI) line or venipuncture is widely used for the treatment of millions of patients around the world [1]. Injections of drugs, liquids, blood products, and Intravenous nutritional supplements are the most important use of these catheters [2]. About 70% of patients need at least one PI catheter after hospital admission, and about 200 million catheters are used per year in the U.S. [3]. But this method is not entirely safe and has some complications. One of these complications is phlebitis which may be present in 50% of the patients in general and up to 75% in patients with infectious diseases, but in patients with no diabetes, burns, or catheterization in emergencies, the incidence is approximately 20% [4].
Phlebitis can be dangerous because it causes clot formation within veins and occurrence of thrombophlebitis and, in some cases, embolism [5]. Another serious complication is sepsis, which occurs in about 1% of cases [3, 6, 7]. Other complications such as drug and fluid leakage, occlusion, and local infection may also be observed [6].
These complications may occur at various stages, during the initial assessment to find the appropriate site for catheterization or subsequently during catheter insertion or maintenance of catheter placement. Several factors affect the incidence of these complications such as aging, gender, vein selection, equipment selection, disease process, treatment protocols, and the skill of the person who performs venipuncture [8].
Catheter site and indwell time are also related to the incidence of complications, especially phlebitis [1, 8, 9]. Hence, although it may take up to one week or even more for catheters and Intravenous fluid administration, they are usually replaced in shorter intervals to minimize the complications [3]. The recommended time interval for routine replacement of catheters has been increased over the past three decades from 24 to 48 hours and then to 72 hours [6]. In some recent nursing studies, the recommended time line is 72 hours [10-12]. In spite of this recommendation, complications sometimes occur sooner. Thus catheter replacement is necessary, and sometimes it is replaced in 72 hours without a complication. The Centers for Disease Control and Prevention (CDC) has recommended this time to every 72-96 hours [13].
The nursing team is responsible for PI catheter insertion and care [14]. Therefore, the determination of complications and their frequencies extent are necessary for nursing care. In this regard, a study conducted in Turkey showed that the incidence of phlebitis in catheterizations, which were in place less than 48 hours, was significantly higher than that of other time durations [9]. Another study on patients admitted to the general surgery department showed that the lowest rate of phlebitis was related to 0-24 h timeline [15].
Results of a prospective cohort study in five Italian hospitals indicates that with every 24 h increase in catheter indwell time, the likelihood of phlebitis increases by 5% [1]. While in a retrospective study on the patients hospitalized in a surgical department in the U.S., no difference was reported between complications of catheters indwelled for 72-96 hours and those remained for more than 96 hours [16].
Considering the wide range of factors affecting the complications of PI catheters and the different results regarding the incidence of these complications, further studies are needed to examine the situation and revise the current guidelines. In this regard, this study aimed to investigate the incidence of complications of PI catheterization within 72 hours after insertion.
Materials and Methods
This is an analytical cross-sectional study design conducted on the patients hospitalized in cardiac surgical wards of an educational treatment hospital in Rasht City, Iran after undergoing Coronary Artery Bypass Graft (CABG) operation. These wards were selected because the patients received the same antibiotics after CABG operation. The point is that the injection of some medications can exacerbate the complications of the injection site vein.
The inclusion criteria for the study patients were as follows: needed PI catheter for at least 72 h; had no peripheral vascular diseases (based on the medical records); not received immunosuppressive drugs (based on the medical records); lacked blood infection (based on the medical records), sensitivity to penicillin and antibiotics based on the routine surgical protocol, valvular heart disease; received the same Intravenous (IV) drugs; lacked allergy to adhesive or medical equipment (based on the medical records); and were interested to participate in the study. On the other hand, the exclusion criteria were as follows: change in the type of IV drugs taken during the study, blood transfusion, skin reaction to dressing adhesive on the catheter, and unwillingness to participate in the study.
According to the study of Salgueiro-Oliveira et al. where the rate of phlebitis was reported 11.09%, a sample size of 154 was determined, and the patients were gradually included in the study based on convenience sampling method [17]. Of 289 patients, 117 did not meet the inclusion criteria: 1 for unwillingness to participate; 75 for not receiving the same IV drugs; 7 for sensitivity to penicillin and thus, not receiving antibiotics based on the routine protocol of the surgical ward; 12 for having peripheral vascular disease; 16 for having valvular heart disease; 1 for receiving immunosuppressive drugs and not receiving the same IV drugs; 1 for having a history of allergy to adhesive tape; 1 for having both valvular heart disease and peripheral vascular disease; 1 for having peripheral vascular disease and not receiving the same IV drugs; and 2 for having PI catheters with different sizes. Of 172 remained patients, 4 patients were excluded as their information about catheter removal was not recorded; 7 patients due to change in the received IV drugs, and 7 patients because of blood transfusion. Thus the information of 154 patients was statistically analyzed.
The data collection tools were phlebitis assessment and infiltration rate scale developed by Infusion Nurses Society (INS) which were mentioned as standard tools to evaluate catheter insertion site in reference Nursing textbooks [5]. The phlebitis assessment scale has been rated from 0 to 4 (0=No signs of phlebitis, 1=pain on the insertion site with erythema or edema, 2=formation of streaks, 3=palpable venous cord with a length of more than 2.5 cm, and finally 4=purulent drainage). The Infiltration rate scale also has a grading scale of 0 to 4 from no sign to white, pale, and semi-translucent skin, tight and leaking skin, swollen and bruised skin, gross edema >15 cm in each direction, deep pitting tissue edema, impaired blood circulation, moderate to severe pain, infiltration of some blood products, and skin irritation and tenderness. Other tools included a form of personal, clinical, and catheter information.
From the beginning of the sampling, the medical records of the patients, who were transferred from the cardiovascular Intensive Care Units (ICUs) to the surgical wards and received new PIs, were investigated in terms of inclusion criteria every day. Each eligible patient was entered into the study only once, and if his or her catheter were removed and replaced with another one, the patient would not be re-entered into the study. In the ICU and during the transfer of the patient to the surgical ward, ICU nurses performed venipuncture according to the conventional method (preparation of the skin with 70% ethanol and fixing the catheter with an IV dressing which is a ready-to-use dressing for the catheter site with an anti-allergy adhesive).
20-Fr catheters (made by B. Braun Medical Inc., Pink color) were used for all patients. The personal, clinical, and catheter information form was completed for each patient and put into his or her medical file. The assessment tools for data collection were also put in each patient’s medical record to help the nurses use them when specifying the reasons for catheter removal. It should be mentioned that before the beginning of the study, the nurses of surgical departments were trained on how to use the study tools and they were asked to use a flexible ruler to measure the edema caused by IV drug infiltration. In case of occlusion of the catheter by a clot, first, they were supposed to aspirate the residual clots from the catheter by a syringe, and in case of failure, remove the catheter. In each working shift, the catheters were examined by the nurses regarding the signs of complications. Whenever the nurses saw any signs of complications, they removed the catheter and recorded the reason and time of removal in the related form.
This study was first approved by the Research Ethics Committee of Guilan University of Medical Sciences (Code: IR.GUMS.REC.1394.51) on May 30, 2015. Then, sampling started from July 28, 2015, and ended on March 18, 2016. The study purpose and procedure were explained to the patients, and written informed consent was obtained from them. They were assured of the confidentiality of their information and were free to leave the study at any time.
The obtained data were analyzed in SPSS V. 22. Descriptive statistics (frequency, mean, and standard deviation) were used for describing the individual characteristics, factors associated with the disease and the characteristics of the catheters. Inferential statistics (Fisher’s exact-test and the Chi-squared test) were used to investigate the effects of complications based on the above data.
Results
Our study results showed that most participants were male, aged over 60 years, and had a BMI of 25-30 kg/m2. Their most common underlying disease was hypertension, followed by hyperlipidemia. Most of the subjects were receiving non-Intravenous anticoagulant drugs (Aspirin, Clopidogrel, Enoxaparin, Warfarin). The most frequently used catheter site was antecubital, and the least frequent site was arm. The indwell time of most of the catheters was 49-72 h; the Mean±SD indwell time was 62.05±24.93 h (Table 1).
Based on the results, 48.7% of patients showed no sign of complications in the catheter site during the first 72 h. After 72 h, catheter replacement was performed according to the instructions of the hospital. About 42.2% of the catheters were removed due to the occurrence of at least one complication where the most common complication was phlebitis followed by an obstruction, drug leakage outside of the catheter, and then drug leakage into the patient’s tissue. Most cases of occurred phlebitis were grade 1 and then grade 2; no patient was observed with grade 3 or 4 phlebitis. All cases of leakage into the tissue were of grade 1 phlebitis (Table 2).
Complications in women were more than men, and the most complications occurred in the period of 25 to 48 hours after the catheterization and the least in the time range of 49 to 72 hours later (22.7%). The results reported a significant relationship between the incidence of complications associated with PIs and gender (P=0.013), indwell time of catheter (P=0.0001), and BMI (P<0.05) (Table 3).
4. Discussion
The results of the current study showed that the most reported complication associated with PI catheterization was phlebitis (grade 1). In the studies of Uslusoy and Mete, and Powell et al. where the measurement scales were similar to those used in the present study, the most commonly reported complication was grade 1 phlebitis as well [15, 18].
In the present study, the incidence of complications between 25 and 48 hours after catheterization was significantly higher than in other periods. Paşalıoğlu and Kaya in their study showed that the rate of phlebitis was significantly different between time groups. The rate was higher in catheterizations that lasted less than 48 hours, and in PI catheter indwelled 49-96 h, the phlebitis rate was lower, where the lowest rates were for catheters that remained for 97-120 hours [9]. Our study result is consistent with theirs. Half of the subjects in our study also had no complications 72 hours after catheter insertion, and the only reason for the catheter replacement was complying with the guidelines to replace any catheters even uncomplicated ones after 72 h.
Some studies have different outcomes. In the study of Van Donk et al. the incidence of phlebitis or obstruction was significantly different in days 1 to 7, but there was no schedule for the increase or decrease of their incidence over time [19]. Powell et al. reported a significant relationship between the incidence of phlebitis and PI catheter indwell time. The phlebitis rate increased from day 1 to 3; from 1.5% in the first day or sooner to 3.2% for two days and 11.7% for three days, but it decreased from the fourth day [18].
In Cicolini et al. study, the results indicate that with every 24-hour increase in indwell time, the likelihood of phlebitis increases by 5%, and the frequency of phlebitis in patients with catheters remaining for 96-120 h is greater [1]. This discrepancy in results can be due to the differences in the clinical characteristics of samples and the properties of the used catheters. In the mentioned studies, the patients with various diseases were included in the study, and the catheters were of different materials and sizes. The types of received solutions and drugs were not the same, and skin preparation was carried out in different ways. All of these factors can affect the incidence of complications. In the current study, these factors were under control.
Some studies have different outcomes. In the study of Van Donk et al. the incidence of phlebitis or obstruction was significantly different in days 1 to 7, but there was no schedule for the increase or decrease of their incidence over time [19]. Powell et al. reported a significant relationship between the incidence of phlebitis and PI catheter indwell time. The phlebitis rate increased from day 1 to 3; from 1.5% in the first day or sooner to 3.2% for two days and 11.7% for three days, but it decreased from the fourth day [18].
In Cicolini et al. study, the results indicate that with every 24-hour increase in indwell time, the likelihood of phlebitis increases by 5%, and the frequency of phlebitis in patients with catheters remaining for 96-120 h is greater [1]. This discrepancy in results can be due to the differences in the clinical characteristics of samples and the properties of the used catheters. In the mentioned studies, the patients with various diseases were included in the study, and the catheters were of different materials and sizes. The types of received solutions and drugs were not the same, and skin preparation was carried out in different ways. All of these factors can affect the incidence of complications. In the current study, these factors were under control.
In this study, the incidence of complications was significantly higher in women, which is consistent with most studies such as Paşalıoğlu and Kaya, Ascoli et al., and Van Donk et al. [9, 16, 19]. In the study of Wallis et al. the incidence of phlebitis and obstruction was also significantly higher in women [20]. Differences in the skin structure of women and men, as well as the difference in the dosage of medications and their underlying diseases, may be the reasons for this discrepancy.
In this study, catheters should be assessed in each working shift concerning the complications. Since the use of the same examiner to check the site of catheters was not possible in three shifts, this task was done by nurses in the surgical wards. Before the study, the study instruments were provided to the nurses and they were trained how to use them. However, the individual differences in how each person uses the tool are involved in determining and rating the complication that may affect the research results. Moreover, it was not possible to use the same adhesive dressing for all the study samples which can affect the results.
Based on the study results, the incidence of PI catheter complications on the third day after insertion was less than that on the first and second days. Considering that different studies have achieved controversial results, further studies are recommended to reach the certainty about the appropriate time for replacement of PI catheters and increasing the routine replacement time for uncomplicated ones.
Ethical Considerations
Compliance with ethical guidelines
This study was first approved by the Research Ethics Committee of Guilan University of Medical Sciences (Code: IR.GUMS.REC.1394.51). The study purpose and procedure were explained to the patients, and written informed consent was obtained from them. They were assured of the confidentiality of their information and were free to leave the study at any time.
Funding
The present paper was extracted from the master thesis of the first author, in School of Nursing and Midwifery, , Guilan University of Medical Sciences.
Authors' contributions
All authors contributed in designing, running, and writing all parts of the research.
Conflict of interest
The authors declared no conflict of interest.
Acknowledgments
Authors would like to thank Deputy of Research, Social Determinants of Health Research Center, Faculty of Nursing and Midwifery of Shahid Beheshti University in Rasht, the respected nurses in surgical wards and cardiac ICUs of Dr. Heshmat Hospital.
References
Khosravi A, Ahmadzade Kh, Arastupor SH,Tahmasbi R. [Check the readability level of health literacy and educational resources available to diabetic patients referred to health centers in Shiraz (Persian)]. Journal of Library and Information. 2014; 16(3):37-57.
Madah M. [The factors associated with adult obesity in Iran: A review (Persian)]. Iranian Journal of Nutrition Sciences & Food Technology. 2012; 7(1):119-27.
Shakeri M , Mojtahedi Y, Naserian J, Moradkhani M. [Obesity among female adolescents of Tehran schools (Persian)]. Payavard Salamat.2012; 6(5):403-11.
Kelly T, Yang W, Chen CS, Reynolds K, He J. Global burden of obesity in 2005 and projections to 2030. International Journal of Obesity. 2008; 32(9):1431-7. [DOI:10.1038/ijo.2008.102] [PMID]
Veghari G, Sedaghat M, Joshaghani H, Hoseini A, Niknezhad F, Angizeh A, et al. The prevalence of obesity and its related risk factor in the north of Iran in 2006. Journal of Research in Health Sciences. 2010; 10(2):116-21.
Rssner S. Obesity: The disease of the twenty-first century. International Journal of Obesity. 2002; 26:S2-S4. [DOI:10.1038/sj.ijo.0802209] [PMID]
Mohammadi M, MahmoodiDarvishani S, Mirzaei M, Bahrololoomi Z, Sheikhi A, Bidbozorg H, et al. [The prevalence of overweight and obesity among dental students Yazd University of Medical Sciences of Yazd in 2014 (Persian)]. Journal of Rafsanjan University of Medical Sciences. 2015; 14(3):189-98.
Tofigi A, BaBai S. [The effect of 12 weeks aerobic exercise training on depression indices and lipid profiles in obese women (Persian)]. Journal of Urmia Nursing and Midwifery Faculty. 2015; 13(2):154-62.
Yahi M, Samadanian F, Hossaini M, Azadbakht L. [Prevalence of overweight and obesity on medical students (Persian)]. Health System Research Journal. 2013; 9(4):421-9.
Mohtasham Amiri Z, Maddah M. [Prevalence of overweight and obesity among female medical students in Guilan-2003 (Persian)]. Iranian Journal of Endocrinology and Metabolism. 2006; 8(2):157-62.
Pasdar Y, Moridi S, Najafi F, Niazi P, Heidary M. [The effect of nutritional intervention and physical activities on weight reduction (Persian)]. Journal of Kermanshah University of Medical Sciences. 2012; 15(6):427-35.
Massey PM, Prelip M, Calimlim BM, Quiter ES, Glik DC. Contextualizing an expanded definition of health literacy among adolescents in the health care setting. Health Education Research. 2012; 27(6):961-74. [DOI:10.1093/her/cys054] [PMID] [PMCID]
Paiva D, Silva S, Severo M, Ferreira P, Santos O, Lunet N, et al. Cross-cultural adaptation and validation of the health literacy assessment tool METER in the Portuguese adult population. Patient Education and Counseling. 2014; 97(2):269-75. [DOI:10.1016/j.pec.2014.07.024] [PMID]
Javadzade H. Health literacy among adults in Isfahan, Iran. Health System Research Journal. 2013; 9(5):540-9. [DOI:10.18502/jchr.v7i4.268]
Lee SY, Tsai TI, Tsai YW, Kuo KN. Health literacy, health status, and healthcare utilization of Taiwanese adults: Results from a national survey. BMC Public Health. 2010; 10:614. [DOI:10.1186/1471-2458-10-614] [PMID] [PMCID]
Tokuda Y, Doba N, Butler JP, Paasche-Orlow MK. Health literacy and physical and psychological wellbeing in Japanese adults. Patient Education and Counseling. 2009; 75(3):411-7. [DOI:10.1016/j.pec.2009.03.031] [PMID]
Esna Ashari, Pirdehgh A, Rajabi F, Sayarifard A, Ghadirian L, Rostami N, et al. [The study of health literacy of staff about risk factors of chronic diseases in 2014 (Persian)]. Scientific Journal of Hamadan University of Medical Sciences. 2015; 22(3):248-54.
Tehrani Bani Hashemi A, Amirkhani MA, Haghdoost AA, Alavian M, Asgharifard H, Baradaran H, etal. [Health literacy in 5 provinces and influencing factors (Persian)]. Journal of Education Development Center. 2007; 4(1):1-9.
Sørensen K, Van den Broucke S, Fullam J, Doyle G, Pelikan J, Slonska Z, et al. Health literacy and public health: A systematic review and integration of definitions and models. BMC Public Health. 2012; 12:80. [DOI:10.1186/1471-2458-12-80] [PMID] [PMCID]
Berkman ND, Davis TC, McCormack L. HealthLiteracy: What is it? Journal of Health Communication. 2010; 15(Suppl. 1):9-19. [DOI:10.1080/10810730.2010.499985] [PMID]
In this study, catheters should be assessed in each working shift concerning the complications. Since the use of the same examiner to check the site of catheters was not possible in three shifts, this task was done by nurses in the surgical wards. Before the study, the study instruments were provided to the nurses and they were trained how to use them. However, the individual differences in how each person uses the tool are involved in determining and rating the complication that may affect the research results. Moreover, it was not possible to use the same adhesive dressing for all the study samples which can affect the results.
Based on the study results, the incidence of PI catheter complications on the third day after insertion was less than that on the first and second days. Considering that different studies have achieved controversial results, further studies are recommended to reach the certainty about the appropriate time for replacement of PI catheters and increasing the routine replacement time for uncomplicated ones.
Ethical Considerations
Compliance with ethical guidelines
This study was first approved by the Research Ethics Committee of Guilan University of Medical Sciences (Code: IR.GUMS.REC.1394.51). The study purpose and procedure were explained to the patients, and written informed consent was obtained from them. They were assured of the confidentiality of their information and were free to leave the study at any time.
Funding
The present paper was extracted from the master thesis of the first author, in School of Nursing and Midwifery, , Guilan University of Medical Sciences.
Authors' contributions
All authors contributed in designing, running, and writing all parts of the research.
Conflict of interest
The authors declared no conflict of interest.
Acknowledgments
Authors would like to thank Deputy of Research, Social Determinants of Health Research Center, Faculty of Nursing and Midwifery of Shahid Beheshti University in Rasht, the respected nurses in surgical wards and cardiac ICUs of Dr. Heshmat Hospital.
References
Khosravi A, Ahmadzade Kh, Arastupor SH,Tahmasbi R. [Check the readability level of health literacy and educational resources available to diabetic patients referred to health centers in Shiraz (Persian)]. Journal of Library and Information. 2014; 16(3):37-57.
Madah M. [The factors associated with adult obesity in Iran: A review (Persian)]. Iranian Journal of Nutrition Sciences & Food Technology. 2012; 7(1):119-27.
Shakeri M , Mojtahedi Y, Naserian J, Moradkhani M. [Obesity among female adolescents of Tehran schools (Persian)]. Payavard Salamat.2012; 6(5):403-11.
Kelly T, Yang W, Chen CS, Reynolds K, He J. Global burden of obesity in 2005 and projections to 2030. International Journal of Obesity. 2008; 32(9):1431-7. [DOI:10.1038/ijo.2008.102] [PMID]
Veghari G, Sedaghat M, Joshaghani H, Hoseini A, Niknezhad F, Angizeh A, et al. The prevalence of obesity and its related risk factor in the north of Iran in 2006. Journal of Research in Health Sciences. 2010; 10(2):116-21.
Rssner S. Obesity: The disease of the twenty-first century. International Journal of Obesity. 2002; 26:S2-S4. [DOI:10.1038/sj.ijo.0802209] [PMID]
Mohammadi M, MahmoodiDarvishani S, Mirzaei M, Bahrololoomi Z, Sheikhi A, Bidbozorg H, et al. [The prevalence of overweight and obesity among dental students Yazd University of Medical Sciences of Yazd in 2014 (Persian)]. Journal of Rafsanjan University of Medical Sciences. 2015; 14(3):189-98.
Tofigi A, BaBai S. [The effect of 12 weeks aerobic exercise training on depression indices and lipid profiles in obese women (Persian)]. Journal of Urmia Nursing and Midwifery Faculty. 2015; 13(2):154-62.
Yahi M, Samadanian F, Hossaini M, Azadbakht L. [Prevalence of overweight and obesity on medical students (Persian)]. Health System Research Journal. 2013; 9(4):421-9.
Mohtasham Amiri Z, Maddah M. [Prevalence of overweight and obesity among female medical students in Guilan-2003 (Persian)]. Iranian Journal of Endocrinology and Metabolism. 2006; 8(2):157-62.
Pasdar Y, Moridi S, Najafi F, Niazi P, Heidary M. [The effect of nutritional intervention and physical activities on weight reduction (Persian)]. Journal of Kermanshah University of Medical Sciences. 2012; 15(6):427-35.
Massey PM, Prelip M, Calimlim BM, Quiter ES, Glik DC. Contextualizing an expanded definition of health literacy among adolescents in the health care setting. Health Education Research. 2012; 27(6):961-74. [DOI:10.1093/her/cys054] [PMID] [PMCID]
Paiva D, Silva S, Severo M, Ferreira P, Santos O, Lunet N, et al. Cross-cultural adaptation and validation of the health literacy assessment tool METER in the Portuguese adult population. Patient Education and Counseling. 2014; 97(2):269-75. [DOI:10.1016/j.pec.2014.07.024] [PMID]
Javadzade H. Health literacy among adults in Isfahan, Iran. Health System Research Journal. 2013; 9(5):540-9. [DOI:10.18502/jchr.v7i4.268]
Lee SY, Tsai TI, Tsai YW, Kuo KN. Health literacy, health status, and healthcare utilization of Taiwanese adults: Results from a national survey. BMC Public Health. 2010; 10:614. [DOI:10.1186/1471-2458-10-614] [PMID] [PMCID]
Tokuda Y, Doba N, Butler JP, Paasche-Orlow MK. Health literacy and physical and psychological wellbeing in Japanese adults. Patient Education and Counseling. 2009; 75(3):411-7. [DOI:10.1016/j.pec.2009.03.031] [PMID]
Esna Ashari, Pirdehgh A, Rajabi F, Sayarifard A, Ghadirian L, Rostami N, et al. [The study of health literacy of staff about risk factors of chronic diseases in 2014 (Persian)]. Scientific Journal of Hamadan University of Medical Sciences. 2015; 22(3):248-54.
Tehrani Bani Hashemi A, Amirkhani MA, Haghdoost AA, Alavian M, Asgharifard H, Baradaran H, etal. [Health literacy in 5 provinces and influencing factors (Persian)]. Journal of Education Development Center. 2007; 4(1):1-9.
Sørensen K, Van den Broucke S, Fullam J, Doyle G, Pelikan J, Slonska Z, et al. Health literacy and public health: A systematic review and integration of definitions and models. BMC Public Health. 2012; 12:80. [DOI:10.1186/1471-2458-12-80] [PMID] [PMCID]
Berkman ND, Davis TC, McCormack L. HealthLiteracy: What is it? Journal of Health Communication. 2010; 15(Suppl. 1):9-19. [DOI:10.1080/10810730.2010.499985] [PMID]
Article Type : Research |
Subject:
General
Received: 2019/06/18 | Accepted: 2019/06/18 | Published: 2019/06/18
Received: 2019/06/18 | Accepted: 2019/06/18 | Published: 2019/06/18
Send email to the article author
| Rights and permissions | |
 | This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |